Understanding Sperm Donation: How the Process Works, Who Can Donate, and What to Expect
Sperm donation has become an important way to help individuals and couples start families while advancing reproductive science. This article explores how sperm donation works today—from donor screening and eligibility to ethical considerations and storage innovations. Whether you’re curious about becoming a donor or simply want to understand the process, learn how modern sperm banks maintain safety, privacy, and accessibility for everyone involved. Discover the latest insights on compensation, consent, and global donation trends shaping the future of fertility options.
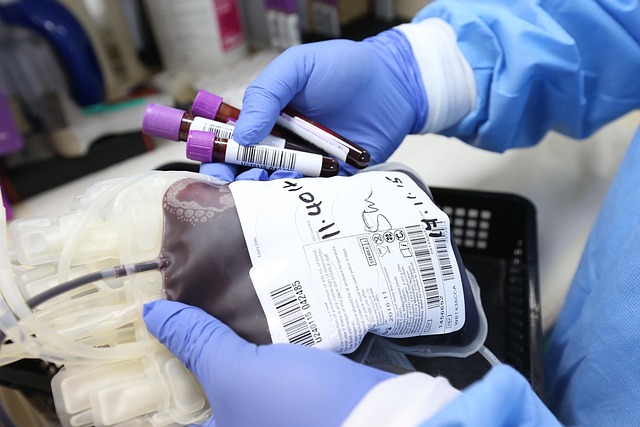
Sperm donation involves providing sperm samples to licensed fertility clinics or sperm banks, where they are processed, tested, and stored for use in assisted reproductive procedures. The process requires significant commitment from donors, typically spanning several months to over a year, with regular donations and comprehensive health monitoring throughout the participation period.
Understanding Who Can Become a Sperm Donor
Becoming a sperm donor involves meeting strict eligibility criteria established by fertility clinics and regulatory agencies. Most facilities require donors to be between 18 and 39 years old, though some programs accept candidates up to age 44. Height requirements typically range from 5’7” to 6’4”, and donors must maintain a healthy BMI between 18.5 and 29.
Educational requirements often include completion of high school, with many programs preferring college-educated candidates. Comprehensive medical and psychological evaluations assess physical health, mental wellness, and family medical history extending back three generations. Genetic testing screens for hereditary conditions, while lifestyle factors such as smoking, drug use, and sexual history undergo thorough review.
Privacy and Confidentiality in Sperm Donation
Confidentiality protocols vary significantly between anonymous and known donation arrangements. Traditional anonymous donations maintain strict privacy barriers, with identifying information kept confidential from recipient families. However, many programs now offer identity-release options, allowing adult offspring to access donor contact information after reaching age 18.
Donor privacy protection includes secure storage of personal information, limited access to identifying details, and careful screening of recipient communications. Some facilities provide coded identification systems, allowing recipients to select donors based on physical characteristics and background information without revealing names or specific locations.
Legal frameworks surrounding donor anonymity continue evolving, with some jurisdictions moving toward greater transparency and offspring rights to genetic information. Potential donors should understand their program’s specific privacy policies and any future obligations or contact possibilities.
Why People Choose to Donate Sperm
Motivations for sperm donation vary widely among participants, with many citing desires to help others build families as primary drivers. Financial compensation, while not the sole motivator for most donors, provides additional incentive for the time and commitment required throughout the process.
Some donors appreciate the comprehensive health screening benefits, gaining detailed insights into their genetic profiles and overall wellness through extensive medical evaluations. Others value contributing to medical research and advancing reproductive science through their participation in fertility programs.
Personal experiences with infertility, either directly or through family members, often inspire individuals to become donors. The opportunity to make meaningful differences in others’ lives while contributing to scientific advancement appeals to many participants seeking purposeful engagement with their communities.
| Sperm Bank | Compensation Range | Requirements | Key Features |
|---|---|---|---|
| California Cryobank | $100-$200 per donation | College education, 5’9” minimum height | Extensive donor profiles, international shipping |
| Fairfax Cryobank | $75-$150 per donation | High school completion, detailed medical history | Photo matching services, genetic counseling |
| Seattle Sperm Bank | $75-$125 per donation | Age 18-35, comprehensive health screening | Identity-release options, ongoing support |
| Xytex Corporation | $50-$100 per donation | College preferred, strict health requirements | Research partnerships, advanced genetic testing |
Compensation rates mentioned are estimates based on available information and may vary by location and individual qualifications. Independent research is advised before making financial decisions.
Global Trends and Regulations in Sperm Donation
International approaches to sperm donation regulation demonstrate significant variation in policies, compensation structures, and anonymity requirements. European countries like Denmark and the Netherlands maintain well-established donation programs with standardized protocols, while nations such as Germany and Italy impose stricter limitations on assisted reproductive technologies.
Emerging trends include increased demand for diverse donor populations, reflecting changing demographics and family structures seeking fertility assistance. Technology advances enable better genetic screening, improved sample processing, and enhanced matching capabilities between donors and recipients.
Regulatory frameworks continue evolving to address ethical considerations, offspring rights, and medical safety standards. Some jurisdictions implement donor limits to prevent excessive biological relationships within communities, while others focus on comprehensive health monitoring and long-term follow-up protocols.
Preparing to Become a Sperm Donor: What to Know
Preparation for sperm donation begins with lifestyle modifications to optimize sample quality and overall health. Recommended changes include maintaining regular exercise routines, following balanced nutrition plans, and avoiding substances that may impact fertility such as tobacco, excessive alcohol, and recreational drugs.
Medical preparation involves completing comprehensive health questionnaires, undergoing physical examinations, and providing detailed family medical histories. Psychological evaluations assess mental health stability and understanding of donation implications, including potential future contact with offspring.
Time commitments require careful consideration, as donation programs typically expect regular visits over extended periods. Most facilities require donations 1-3 times weekly for 6-12 months, with additional appointments for testing and evaluations. Understanding these obligations helps potential donors make informed decisions about participation.
Sperm donation represents a significant commitment requiring careful consideration of personal, medical, and ethical factors. Potential donors should thoroughly research programs, understand legal implications, and consider long-term consequences before beginning the application process. This meaningful contribution to reproductive medicine helps countless individuals and families achieve their parenting goals while advancing scientific understanding of human fertility.




